The Digital Disruption in Diabetes Care
"Diabetes", The word and an article on the condition feel like an unwanted sequel to a movie that you have already seen. In the past decade, there have been innumerable articles on diabetes, the risk factors, how to manage it, how to live with it and even how to cure it. But there seems to be no end in sight to the diabetes epidemic or the articles and news bytes that highlight it.
So why is this disease the focus of so many articles, doctors, policymakers and governments? Is it really as bad as it is portrayed in the media? Why is it important for any of us to invest time and effort in understanding this disease? These are some of the questions that we will try to answer in this article (without going into the technicalities) as we try to demystify the disease and its complications. Specifically, we will look at how diabetes is important to the Indian population.
NO ONE IS REALLY SAFE
Now as far as titles go this one is pretty ominous and we don't mean to start a panic (especially post-COVID which has left all of us jittery and nervous), but it is important to stress that diabetes can occur in everyone and at any stage in life. We won't bore you with the textbook details on the types of diabetes and their modes of affecting our bodies, but of the two main types (type 1 and type 2), that is of concern to us Type 2 diabetes is often caused by lifestyle factors like eating too much sugar and having a sedentary lifestyle. Type 1 or diabetes Mellitus is more of a bad inheritance thanks to the faulty genes (like a bad loan passed down to you by your parents) and is not really reversible. People who suffer from Type 1 diabetes are in it for the long haul and will need medication for the rest of their lives.
However, we have found through meticulous research that type 2 diabetes can not just be managed but can be made to go into remission through, you guessed it, lifestyle changes. It seems the cause and cure for this disease are the same and that can be a bit confusing for anyone. Now if you have read this far there are probably many of you wondering why this has anything to do with you, after all, you exercise regularly, are thin, fit and don't really have any belly fat. Surely the disease is for the fat people, the smokers, the alcoholics and the binge eaters to worry about? The surprising answer is NO. At least if you belong to the Indian ethnicity and population it is.
Some heads are probably turning at this statement that thin people are just as much at risk of developing type 2 diabetes as those who are much heavier and have a much higher BMI. BMI (Body mass index) has been the favourite way of doctors to measure the susceptibility of patients to not just diabetes but a host of other diseases as well. School children learn ( at least I did, textbooks may have changed in the last 15 years) about BMI and how a value over 25 is considered undesirable and 29-35 was categorized as "morbidly obese". But through repeated observations and studies we have found that this logic doesn't apply to Indians in general. India has one of the highest diabetes burdens in the world, it is estimated that about 77 million people had type 2 diabetes in India as of 2019 and that number is only projected to grow.
WHAT IS DIFFERENT FOR INDIAN POPULATIONS?
The money question as they say is definitely what is different about our Indian populations? Is it our genetics? Our diet? Our lifestyle? Our nutrition.? Turns out, it's a little bit of all of them. The standard BMI measurements can be misleading in the case of Indians, it was found in a multi-ethnic study conducted in the UK that an Indian with a BMI of 22 had the same diabetes risk as a white man with a BMI of 30. Those numbers are quite shocking! A BMI of 22 is that of a thin, fit and robust person, how can such a person have the same risks as a man who is quite clearly in the very obese category? Turns out that this same question stumped quite a few researchers, in fact, Dr Yajinik who has worked for decades in the field published a paper called "Confessions of a thin-fat Indian" that highlights his journey in the field and how he found out that what most studies missed out because they focused on white populations.
It has been found that not just Indians but south-east Asians are all part of the group to which these new parameters apply. As a doctor, it can be quite confusing when you have been taught since medical school that it is the overweight people with unhealthy lifestyles that get the disease, but in your practice, you see thin and sometimes emaciated people, young mothers who are suffering from the disease. This seems illogical, but there is a reason behind this. The theory behind this is called the "Thrifty gene hypothesis" which suggests that we as humans evolved to survive through periods of starvation and abundance but these days with the ready availability of food our starvation phase adaptations are not really necessary, but they work anyways and this can lead to the insulin resistance that is seen in diabetics. This is one of several explanations given by doctors and researchers but it doesn't answer all the questions.
IS OUR DIET A CULPRIT?
The burning question on many of your minds is probably, Is my diet putting me at risk? The answer is yes, our Indian diet and our palates can be very varied but for large parts of the country, all meals are heavy in complex carbohydrates, namely rice. The South Indian states in particular enjoy a wide variety of dishes that are rice based and these carbs can be a big contributor to developing insulin resistance and diabetes. This is a common pattern across Southeast Asian countries such as Sri Lanka, Thailand, Cambodia, Burma, Philippines, etc where carb-heavy meals are the norm.
This means that these populations are at risk for early onset diabetes and for getting type 2 diabetes in people with normal BMIs. The comparative risk is that thirty-year-old thin people have the same risk of getting diabetes as old white people who are obese. This is worrying especially because for a large section of the population in countries like India, what they eat is dictated by how much they earn and the availability of diverse food products. There is a disturbing trend that has been observed of women who were undernourished during pregnancy having children who are primed even before birth to be diabetic, which they can then pass on to their children.
Imagine a mother from a poor socioeconomic background who is not getting adequate calories during her pregnancy, the child makes up for the lack of nutrients by developing a coping mechanism that can lead to insulin resistance in them. This is called MRDM (Malnutrition related diabetes mellitus), and in fact, this type of diabetes is recognized by the WHO as one of the major types in the world but especially among Indian populations. There are studies published in the early 90s that point the finger at low birth weight as a cause of type 2 diabetes.
IN A NUTSHELL
As you have read through this article you would have certainly noticed that the risk factors, age and nutrition criteria, all seem pretty stacked against Indian and Southeast Asian populations. We are at greater risk of:
- Getting diabetes earlier
- Having a normal BMI and still having the disease
- Can develop risk factors even in the womb
- Our diets and staple foods can increase our chances of getting the disease.
In such a scenario what are the steps available to us? We cannot change the diet of a billion people, nor can we solve the issues of poverty and hunger in our country overnight. Type 2 diabetes in particular has a very high percentage of remission, given that there is a change in lifestyle habits, weight loss, exercise patterns, etc. But how do thin people lose more weight? This was the question posed by doctors all over the country when these findings came to light, regularly prescribing medications or advising bariatric surgery is not a sustainable treatment method.
So to deal with affects such a large section of the population, we need a coordinated and concerted effort from the healthcare industry and from the policymakers in the government.
A DIGITAL REVOLUTION
Conventional changes take time and with a large population such as the one in India, providing coverage for health-related issues has always come with its own set of challenges. It is a logistical nightmare to track the diabetic status of such a large number of people and to store and analyze that data. The funding required for that would be huge and let's face it, such a project that requires so much money and manpower would be abandoned halfway due to any number of reasons.
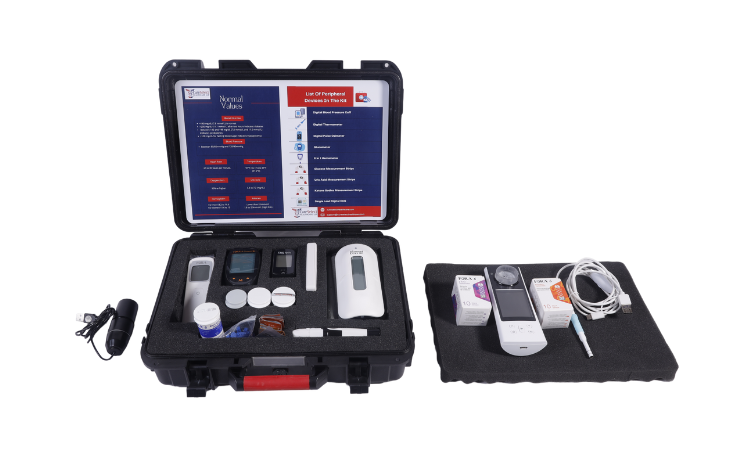
But the good news is that the private sector in the healthcare industry has already launched an effort at increasing awareness about the disease amongst the public and also expanding the treatment and therapy options available to them. The latest and perhaps most significant weapon in this arsenal is Digital healthcare and Telemedicine. By using simple software applications that can work on any smartphone it becomes quite simple to gather the healthcare data of people across the country. The rise in remote monitoring devices such as at-home glucometers and haemometers means that patients can monitor the levels of their blood sugar by themselves and that data is available to their doctors in real-time.
Monitoring pregnant mothers, those already suffering from type 2 diabetes and a host of other things become simplified with the use of Telehealth services:
- Continuous patient monitoring
- Prescribing medications
- Checking patient compliance
- Monitoring sugar levels remotely
- Identifying at-risk individuals early
- Tracking treatment outcomes
- Maintaining Electronic patient records
- Connecting poor patients with diabetologists
There are many ways in which the digital healthcare model that has become so popular with private hospitals and healthcare providers can be leveraged for the early detection, treatment, counselling and remission monitoring of people suffering from diabetes. This is possible in today's scenario due to the increased penetration of the internet to all parts of the country and also the increased smartphone usage by the average Indian.
Digital health and Telemedicine can help to bridge the gap between the demand and supply of not just doctors, but also nutritionists, counsellors, pharmacists and other specialists to the population that needs them. In a country of vast distances and a deficit in healthcare professionals, digital medicine can help to preempt and prevent the huge burden that this disease places on the population.