7 Reasons to Invest in Telemedicine for your practice
Doctors and medical professionals were among the worst hit during this pandemic. Suffering massive burnouts, continuous work hours, grappling with an unknown and highly infectious pandemic, getting sick themselves were all hallmarks for exhausted and stretched thin medical professionals these past two years. A spill over from this COVID pandemic was patients requiring regular care being unable to access their physicians due to unavailability of beds or fear of infection.
While the big hospitals and chains were struggling to deal with testing, triaging and treating the massive tide of sick or infected small clinics, dental practices, group practices, psychiatrists, dieticians, counsellors and other medical practitioners with local & small scale practices were affected in quite a different way.
How Your Neighbourhood Practice Matters
Many a time when the words national healthcare or healthcare budget are mentioned our minds immediately bring up the images of multi story hospitals or crowded public hospitals that cater to large swathes of the population. However the true reach of comprehensive medical and dental care lies in the local clinics, small scale practices since they grow along with their communities and are more in touch with the needs, diseases and issues faced by that community.
Local clinics usually have a closer relationship with their patients since they are usually family based practices where patients can get familiar with the same doctor over time unlike in large private or public institutions where they are usually seen by a floating population of doctors. Small practices depend on building good and sustainable relationships with the patients in their community since their financial viability and survival depend on it.
All this means that many people are more comfortable coming forward with embarrassing health complaints to their regular GP rather than one at a hospital. These local practices are also located much closer in case of emergencies, the doctors are more familiar with the histories, can perform triage and first aid quickly.
Lockdown and the Domino Effects
Many dental, general, stand alone and holistic medicine practices were shuttered as they weren't considered part of the essential services or doctors themselves were afraid of their practice becoming epicentres for Covid. This cut off revenue for all such consulting practices while the operational costs remained the same. Even when various state and the central governments allowed the functioning of clinics, the fear of infection and hesitancy towards vaccine mandates etc made sure that there was only a trickle of patients coming in for consults.
The rent, maintenance, upkeep and the need to adhere to new disinfection and COVID protocols (fumigations, sanitizations, PPE kits, UV sterilization, testing kits and isolation for staff and patients) all drove up operating costs. This has ended up spiralling into a losing scenario for both patients and small practice owners.
Many in the dental. Ayurveda, homeopathic, veterinary fields were vocal that lockdowns should not shutter their small and group practices as long as proper pandemic and patient handling protocols were followed. This was not just to bolster struggling local practices but to also facilitate continuing care for many elective treatments that greatly affect the QOL(Quality of life) of patients.
Technology Provides the Solution
The rise in COVID cases coupled with the orders to quarantine in place, discontinue or put on hold all non emergency medical procedures has seen the rise of alternative modes of healthcare consultation. Phone calls, video consults, group sessions, use of apps and web applications for connecting patients and doctors rapidly gained popularity. Many hospitals, practices and governments depended heavily on and invested in apps to know the COVID status of patients, create channels for patients to reach out to doctors or find emergency resources.
There has been a massive shift towards using Telemedicine and remote consults for a wide variety of cases especially those related to pain care, neurology, psychiatry and long term patients. For physiotherapists, counsellors for depression, stroke, addictions etc a few missed sessions can have drastic impact on the progress and positive changes achieved by the patient. Using Telehealth solutions many patients were saved from a potential backslide.
Pros & Cons
Pros
- Ease of use
- Can connect to multiple patients at once
- Safety and zero chance of infections
- Can schedule at convenience
- Can call in other doctors for a consult easily
- Patients feel comfortable in a familiar environment
- Electronic health records can be viewed in consult just like in person
- Saves time and money, effort and travel for patients
- No need to wait in long lines and crowded waiting rooms thus increasing the chances of infection
Cons
- Connection needs to be secure
- It can be hard to read facial cues on a computer screen
- Online consults can feel impersonal
- Patients can become distracted by others at home
- Hard to make children sit in front of computer screens for long times
- Hard to access for those not well versed in technology
- Internet connectivity and devices are a must and this can be hard to find in third world countries & poor populations
- Problems with payments, billing and insurance pay outs
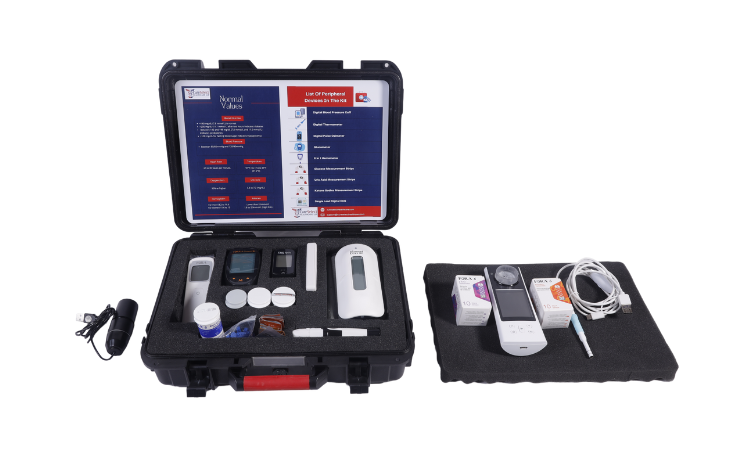
Telemedicine Solutions
The increased need for Telemedicine has led to a greater influx of private players who are coming up with innovative solutions for remote healthcare management and digital healthcare. This is reflected in the sheer number of scheduling and Teleconsultation apps that are now flooding the market. While their premise might be the same they offer unique in app features, ability to create and store electronic patient records, maintain records of patients seen and the diagnoses given etc.
This can be of great benefit to the small and medium community practices especially the ones located in remote locations since they can cheap and easy alternatives to in person consults, thus reducing the burden on both the physician and the patient. It can be an extremely easy to deploy and immensely helpful for poor, old, remote communities.
The ability to remote teleconsult with specialists to arrive at a better diagnosis can be a great boon for both the less experienced/ younger doctors in the field and the patients they care for. Many lives can be saved by timely intervention, early detection thanks to the ability to consult say an oncologist for a breast cancer patient.
All in all though there are several kinks to be worked out especially with regards to privacy, payment gateways, insurance and billing etc, it is still a great idea to invest in a Telemedicine software or service for your clinic/ hospital not just to stay with the times but also to increase the accessibility and adaptability of your practice, thus leading to healthy finances and happy patients.